Puberty blockers are given to children to delay puberty. They can be given to trans/non-binary/genderqueer children to delay or prevent some of the distressing physical changes that take place during puberty. Some children start puberty blockers with the plan of later using hormone replacement therapy (HRT) to further medically transition. Other children use puberty blockers as a way of giving themselves time and space to consider how they'd like to physically express their gender, before the changes happen on their own.
Puberty causes physical changes that are irreversible (or at the very least, require surgery to change). These include (for those with testes) deepened voice, development of an Adam's apple, and (for those with ovaries) breast development.
Puberty blockers' effects are reversible (i.e. puberty will resume when it stops being blocked).
The Endocrine Society has guidelines recommending the use of hormone blockers. They recommend that puberty blockers are used at the first sign of puberty (known as Tanner Stage II).
The Biological Mechanism
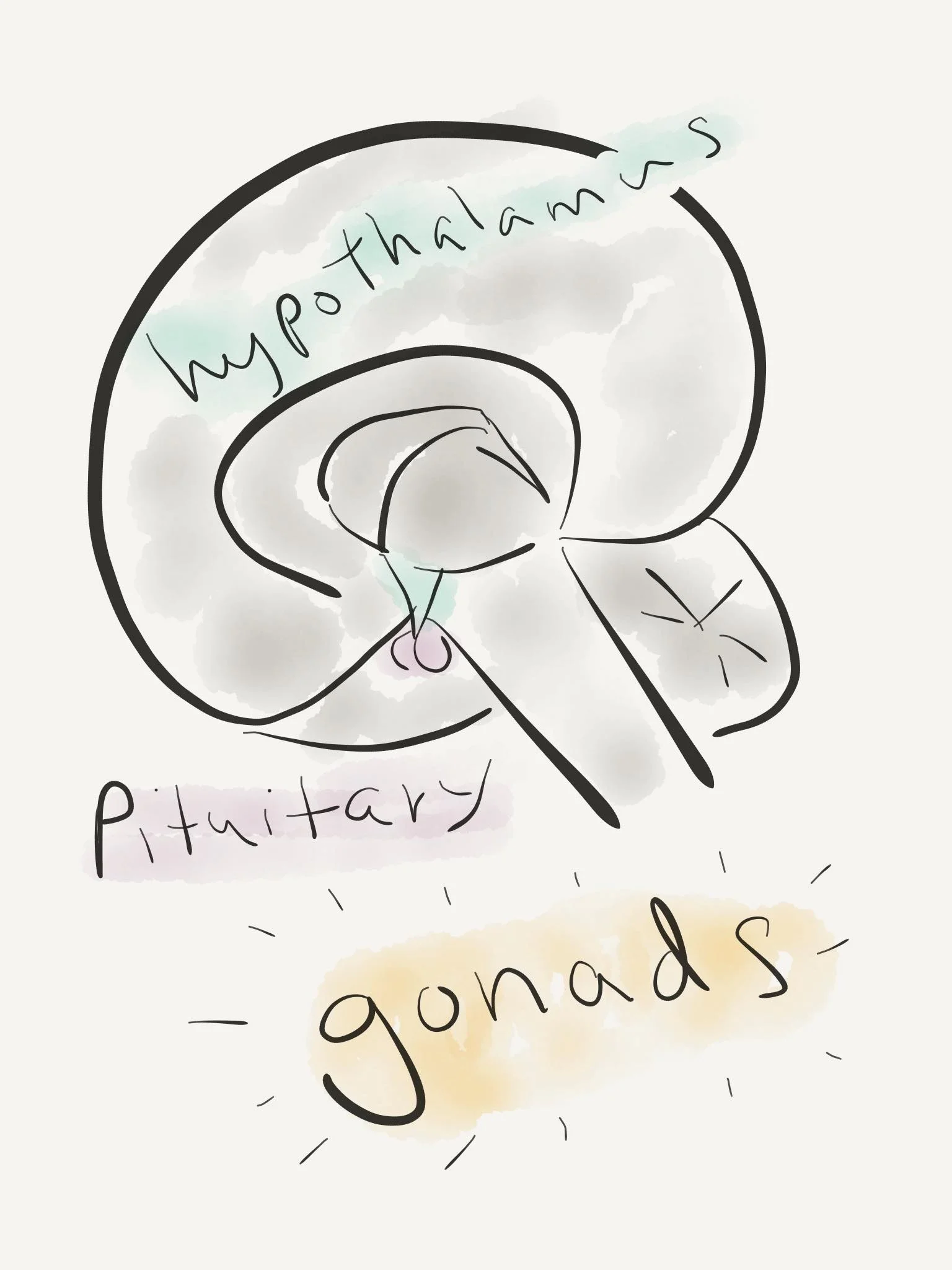
The glands responsible for puberty are known as the HPG axis. This is an endocrine system made of the hypothalamus, the pituitary gland, and the gonads.
This axis is part of a feedback loop that mediates puberty. The glands respond to different messages from each other to alter their own activities.
By changing the messages along this axis, we can pause the mechanism of puberty.
The HPG axis involves a cascade of neurotransmitter signals from one gland to the next.
The messages from the hypothalamus to the pituitary to the gonads.
The hypothalamus sends GnRH (Gonadotropin-releasing hormone) to the pituitary.
The pituitary then sends LH (luteinizing hormone) and FSH (Follicle-stimulating hormone) to the gonads.
The gonads release androgens and estrogens, as well as other feedback messages to the hypothalamus and pituitary.
Androgens are hormones, such as testosterone, responsible for the development of male sex characteristics, such as testicular enlargement. Estrogens are hormones that develop female sex characteristics, such as ovulation.
Normal HPG axis signalling facilitates the physical changes typically seen in puberty.
In unscientific terms, the pituitary doesn't like this. It essentially goes "Where are the bursts I'm used to? What are you doing? I'm out, brah."
The pituitary stops sending out LH and FSH. This breaks the HPG axis's feedback loop. The signals that mediate puberty are halted! Puberty is blocked!
Puberty blockers, such as Lupron, mess with this signaling.
The hypothalamus usually signals the pituitary in bursts. The pituitary interprets the intensity and duration of the GnRH bursts to determine what hormones it sends out.
Lupron floods the pituitary with neurotransmitter signals. Lupron is a GnRH analog, which means that it mimics GnRH. Instead of receiving occasional bursts of neurotransmitters, the pituitary is bombarded with GnRH.
What's next?
After using puberty blockers, some children decide that their gender expression feels less tied to their body and they let their body proceed with puberty however it wants to.
Other children wish to further transition using HRT. This treatment uses what is called "cross-sex hormones."
Cross-sex hormones are estrogen those with testes and testosterone for those with ovaries.
The Endocrine Society guidelines suggest that HRT be started at age 16. This is a suggestion, not a firm rule.
Some doctors will start kids on HRT earlier, depending on various factors. Many doctors use physical and cognitive development in combination with age to assess readiness. The course of puberty takes a while, so children who start HRT earlier are closer to their peer's development. Doctors can also consider factors affecting bone/neurological health.
Below are example HRT courses to be given to patients. The doses are titrated (adjusted) until the person reaches a certain hormone level. For female-to-male transitions, the dose stops being adjusted when the person is in the mid-to-high range of testosterone found in cisgender men (men who identify with the gender they were assigned at birth, also known as bio men/males). For male-to-female transitions, the dose is set when the person has estrogen and testosterone levels equivalent to cisgender women (bio women/females).
Many people continue on these dose levels into the future, only to be adjusted based on feedback from routine blood tests. Some people continue on these doses for awhile, then decide to change their dosage for other reasons.
Gender is a complicated aspect of our identity. Our relationship to and experience of our own gender can change with time and age. My role as a therapist isn't to push clients toward a certain endpoint, but help them fully express and embrace who they are. Life is confusing and messy, but we're not alone.
<3 Vered